Hemodialysis access failures take a great toll on a patient’s quality of life. Frequent hospital admissions, invasive diagnostic tests, and open and endovascular reinterventions are associated with increased morbidity.1 Maintaining vessel patency in hemodialysis patients is critical; however, surgical access durability is temporary at best, with half-life for arteriovenous grafts lasting approximately one year and arteriovenous fistulas providing only slightly better outcomes.1 A common failure of hemodialysis access is stenosis or occlusion of the dialysis outflow circuit. Obstructions caused by cellular migration and tissue accumulation across graft ePTFE layers can be a contributing factor.
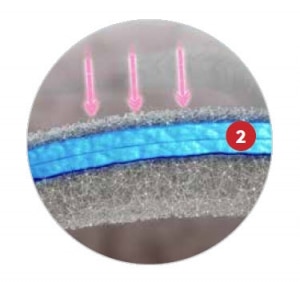
Addressing this clinical challenge, Merit Medical® introduced the Merit WRAPSODY™, a novel endoprosthesis designed with a revolutionary cell-impermeable middle graft layer. With this unique feature, the Merit WRAPSODY Endoprosthesis inhibits transmural cellular migration without the use of drug bonding, helping to prevent obstructions from forming within the endoprosthesis.
To evaluate device performance, Dolmatch et al. published a study 2 in the Journal of Vascular and Interventional Radiology comparing the patency, cellular response, and thrombogenicity of the Merit WRAPSODY with that of a leading ePTFE covered stent. Both Merit WRAPSODY and leading ePTFE covered stent grafts were implanted in the external iliac arteries of 14 adult sheep for 30 (n = 4), 90 (n = 4), and 180 (n = 6) days. Angiographic patency and percent diameter stenosis (%DS) were assessed at termination. Excised stent grafts were fixed and stained for histopathologic analysis, including neointimal coverage (NC) assessment.
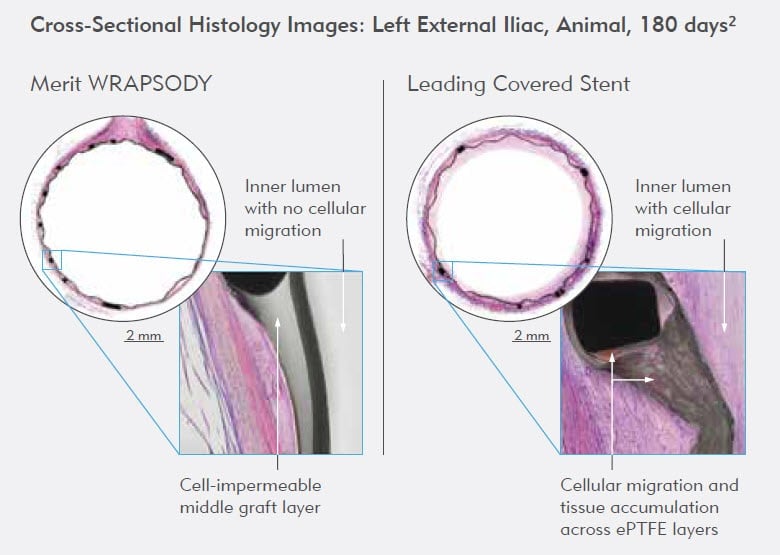
Results showed that the Merit WRAPSODY had lesser mean %DS in comparison to the leading ePTFE covered stent: 4.6% vs. 8.2% (P = .563), 2.0% vs. 10.9% (P = .363), and 2.1% vs. 10.3% (P = .009) at 30, 90, and 180 days, respectively. In addition, median NC scores at 30, 90, and 180 days were significantly lower in middle Merit WRAPSODY sections (P <.05). Proximal and distal Merit WRAPSODY and leading ePTFE covered stent sections exhibited similar median NC scores at all time periods (P >.05).
The authors of the study concluded that the Merit WRAPSODY’s cell-impermeable middle graft layer prevented cellular migration and tissue accumulation across device layers and around nitinol stent struts better than the leading ePTFE covered stent.
In addition to animal models, human trials to investigate the Merit WRAPSODY’s safety and effectiveness are currently underway. The WRAPSODY FIRST, an ongoing clinical trial, will have 6-month and 12-month patency data available at the beginning of next year. Moreover, the WRAPSODY AV Access Efficacy (WAVE) IDE study is expected to start enrolling patients in January 2021. Merit received the CE mark for the Merit WRAPSODY™ from the British Standards Institution (BSI) earlier this year.
Every day Merit works to create solutions to clinical challenges that once seemed impossible. Engineered with dialysis patients in mind, the Merit WRAPSODY Endoprosthesis provides a viable treatment option that preserves functional hemodialysis access.
Discover the Merit WRAPSODY and its many innovative design features by visiting the product page, and contact Customer Service for more information about how you can incorporate the Merit WRAPSODY into your practice.
Related
References
- Rodriguez, Eduardo, et al. 2017. “Hemodialysis Outflow Vein Stenosis.” In Hemodialysis Access Fundamentals and Advanced Management, edited by Sherene Shalhub, Anahita Dua, and Susanna Shin, 257–263. Switzerland: Springer International Publishing.
- Dolmatch, Bart L., John W. Hall, Wayne L. Mower, and Serge D. Rousselle. 2020. “Evaluation of a Novel Spun Polytetrafluoroethylene Stent Graft in an Ovine External Iliac Artery Model.” Journal of Vascular and Interventional Radiology 31: 494–502.